A Comprehensive Guide for Families and Care Facilities
Parkinson’s disease is a progressive neurological disorder that primarily affects movement, balance, and coordination. For care facilities and families supporting older adults, early diagnosis and structured treatment plans are essential to improving quality of life and slowing disease progression.
What Is Parkinson’s Disease?

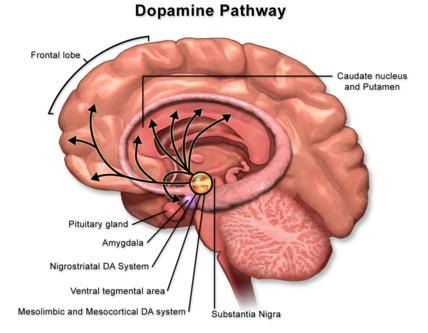
Parkinson’s Disease is a chronic and progressive disorder of the nervous system caused by the loss of dopamine-producing neurons in the brain. Dopamine is essential for smooth, coordinated muscle movements.
Common Early Signs
- Tremors (shaking), usually starting in one hand
- Slowed movement (bradykinesia)
- Muscle stiffness (rigidity)
- Impaired posture and balance
Symptoms often develop gradually, making early detection challenging but critical.
How Parkinson’s Disease Is Diagnosed
Diagnosing Parkinson’s disease is primarily clinical, meaning there is no single definitive test. Instead, healthcare professionals rely on a combination of evaluations.
1. Medical History and Symptom Review
Doctors assess:
- Onset and progression of symptoms
- Family history of neurological disorders
- Medication history
2. Neurological Examination
A specialist evaluates:
- Reflexes and coordination
- Muscle tone and movement
- Gait and balance
3. Response to Medication
Patients may be given medications like Levodopa to observe symptom improvement, which supports diagnosis.
4. Imaging Tests (Supportive, Not Definitive)
- MRI or CT scans may rule out other conditions
- Specialized scans can assess dopamine activity
Treatment Options for Parkinson’s Disease



While there is currently no cure for Parkinson’s disease, treatments focus on managing symptoms and improving daily function.
1. Medications
Medications are the cornerstone of treatment:
- Dopamine replacement drugs (e.g., Levodopa)
- Dopamine agonists to mimic dopamine effects
- MAO-B inhibitors to slow dopamine breakdown
These medications help control tremors, stiffness, and slow movement.
2. Physical Therapy and Rehabilitation
Structured therapy programs help maintain mobility and independence:
- Improve balance and coordination
- Reduce risk of falls
- Enhance muscle strength and flexibility
3. Occupational Therapy
Supports patients in performing daily activities such as:
- Dressing
- Eating
- Bathing
This is especially important in assisted living and long-term care facilities.
4. Speech and Swallowing Therapy
Parkinson’s can affect speech clarity and swallowing ability. Therapy helps:
- Strengthen vocal muscles
- Improve communication
- Reduce choking risks
5. Surgical Treatment
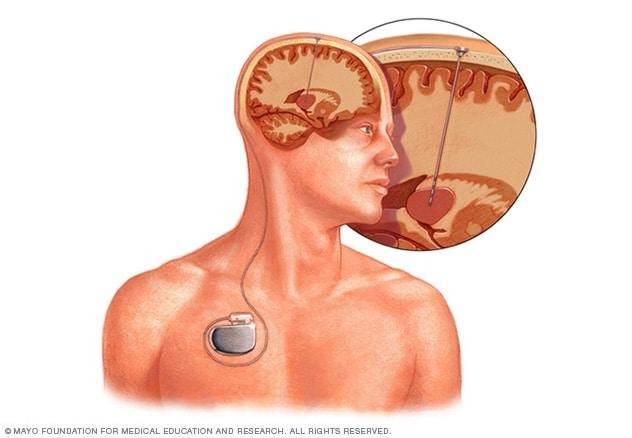
For advanced cases, procedures like Deep Brain Stimulation (DBS) may be recommended:
- Involves implanting electrodes in specific brain areas
- Helps regulate abnormal brain activity
- Reduces severe motor symptoms
The Role of Care Facilities in Parkinson’s Management
Care facilities play a vital role in ensuring consistent, high-quality support for individuals with Parkinson’s disease.
Final Thoughts
Parkinson’s disease presents ongoing challenges, but with early diagnosis and comprehensive treatment, individuals can maintain a meaningful and active life. For families seeking care and facilities providing services, knowledge and consistency are key.

